Behavioral health systems have made significant strides in expanding access to care. Peer services have grown across outpatient clinics, crisis teams, Certified Community Behavioral Health Clinics (CCBHCs), and substance use treatment programs. Telehealth has normalized remote care. Patient portals are widely available.
And yet, engagement remains a persistent challenge.
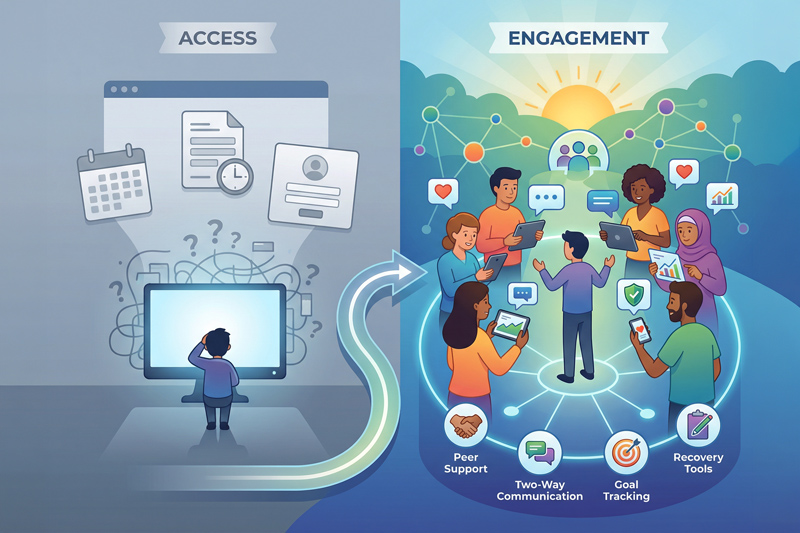
In recent national surveys examining provider perspectives and consumer preferences on digital engagement in behavioral health, one theme emerged consistently across both groups. Access to tools does not automatically translate into meaningful participation in care. Consumers described early experiences with services as administratively heavy, confusing, and impersonal. Providers acknowledged difficulty sustaining engagement during intake and the critical first weeks of treatment. Both groups highlighted the period between visits as a vulnerability point—when motivation can waver, relapse risk can rise, and connection to the care team may feel distant.
These findings suggest that the next phase of behavioral health innovation must focus less on expanding access and more on redesigning the consumer experience itself.
The Consumer Journey: Where Engagement Breaks Down
From the consumer’s perspective, the behavioral health journey often begins with urgency—crisis, distress, substance use relapse, family conflict, or psychiatric decompensation. Yet the first digital touchpoints frequently involve lengthy forms, multiple logins, consent documents, and screening tools delivered without context.
Our survey data revealed that providers see significant drop-off during intake and onboarding. Consumers reported feeling overwhelmed by information, uncertain about next steps, and unsure how to communicate questions between appointments. Traditional portals—when used—are often limited to appointment reminders or document access rather than interactive engagement.
This misalignment matters. Research consistently demonstrates that early engagement predicts retention in treatment, which in turn correlates with improved outcomes in both mental health and substance use disorder care (SAMHSA, TIP 42). Yet digital systems in many organizations were not designed to support sustained, recovery-oriented engagement. They were built for administrative efficiency.
The result is a structural gap where consumers spend most of their time outside clinical settings, but digital infrastructure does little to support continuity during those hours and days.
Between Visits: The 99% Problem
Behavioral health treatment is episodic. Recovery is continuous.
Consumers spend perhaps one hour per week in formal sessions. The remaining time, what might be called the “99% problem,” is when coping strategies are tested, social stressors emerge, cravings fluctuate, and motivation shifts.
In our survey, providers acknowledged that between-visit engagement is difficult to monitor. Consumers expressed interest in tools that would allow them to check in, track goals, communicate securely, and access recovery resources without waiting for the next appointment.
This is not a request for automation. It is a request for connection.
Peer services illustrate this dynamic clearly. Individuals with lived experience often provide crucial support during transitions—after hospitalization, during early recovery from substance use, or when navigating new diagnoses. But from the consumer’s standpoint, peer support is not a separate programmatic silo. It is part of a broader recovery ecosystem.
Digital platforms that fail to integrate these elements into one cohesive experience risk reinforcing fragmentation.
Reframing Digital Engagement as Partnership
If we begin with the consumer experience rather than organizational workflows, a different design philosophy emerges.
Instead of static portals, behavioral health systems can envision collaborative consumer engagement hubs—integrated digital environments that support:
- Recovery-aligned onboarding that introduces services clearly and reduces information overload
- Secure, two-way communication with members of the care team
- Structured mood check-ins and goal tracking that reinforce progress
- Embedded safety planning and harm reduction tools
- Access to peer supports and lived experience guidance
- Navigation assistance for housing, food, transportation, and other social needs
This model shifts digital engagement from passive access to active collaboration.
Importantly, such platforms must reflect recovery-oriented principles articulated by the Substance Abuse and Mental Health Services Administration (SAMHSA), including person-centeredness, empowerment, and strengths-based care. Consumers consistently report that feeling heard and understood matters as much as the clinical intervention itself.
When digital systems reinforce these principles, they extend the therapeutic alliance rather than merely documenting it.
The Role of Peer Services Within a Consumer-Centered Engagement Hub
In a consumer-centered digital ecosystem, peer services become more accessible and visible—not as add-ons, but as integrated supports.
For example:
- A consumer completing a digital check-in that indicates increased anxiety or relapse risk could receive an outreach message from a peer specialist.
- Onboarding materials could include a brief introduction to peer services, demystifying the role early in the journey.
- Recovery milestones tracked digitally could be reinforced by peer encouragement.
- Post-hospital follow-up could include coordinated outreach that blends clinical and peer engagement.
Research on peer support has demonstrated improvements in hope, empowerment, and engagement among individuals with serious mental illness and substance use disorders (Chinman et al., 2014; Solomon, 2004).¹ However, operational barriers—including documentation workflows and siloed communication systems—can limit the scalability of peer services.
When digital infrastructure integrates peer communication within the broader care team workflow, it enhances coordination while preserving role clarity. From the consumer’s perspective, the experience feels cohesive rather than segmented.
Measuring Engagement Meaningfully
As CCBHC expansion continues nationally and value-based payment models evolve, organizations face increasing expectations to demonstrate measurable outcomes, such as follow-up after hospitalization, retention in substance use treatment, and crisis response effectiveness.
Traditional engagement metrics—appointment attendance, portal logins—capture only part of the picture.
A consumer-centered engagement hub offers the opportunity to measure more nuanced indicators:
- Completion rates for digital onboarding
- Response patterns to structured check-ins
- Engagement frequency during the first 30 days of treatment
- Utilization of safety planning tools
- Interaction with peer services within digital workflows
Such data can inform early identification of disengagement risk, allowing proactive outreach rather than reactive response.
Crucially, these metrics should serve improvement, not surveillance. Transparency with consumers about how data is used is essential to maintaining trust.
Equity and Accessibility
Digital innovation must also address disparities in access and usability. Survey respondents noted differences in digital literacy, language accessibility, and device availability.
A next-generation consumer engagement strategy must therefore include:
- Mobile-first design
- Multilingual interfaces
- Clear, plain-language communication
- Accommodation for varying literacy levels
- Optional hybrid models that blend digital and in-person support
Peer services are particularly valuable in bridging digital divides. Individuals with lived experience can guide consumers in navigating platforms, troubleshooting barriers, and integrating tools into everyday life.
Technology alone does not solve inequity, but thoughtfully designed digital infrastructure can reduce friction and expand access when paired with relational support.
Moving Beyond the Traditional Portal
Across the behavioral health field, organizations are recognizing that legacy patient portals are insufficient for the complexity of recovery journeys. In response, some behavioral health technology leaders are developing next-generation consumer engagement hubs within their electronic health record ecosystems.
These platforms aim to integrate communication, structured engagement tools, peer support options, safety planning, and measurable analytics into a unified digital experience. Rather than layering features onto outdated systems, the goal is to design around how consumers move through care.
Such efforts reflect a broader shift from transactional access toward recovery-centered partnership.
Conclusion: Designing for the Recovery Experience
Behavioral health systems have invested heavily in expanding services. The next investment must be in experience.
Our survey findings underscore that consumers want more than appointments and reminders. They want clarity during intake, connection between visits, accessible peer support, and tools that reinforce recovery goals in real time.
A consumer-centered engagement hub—integrated within clinical workflows and oriented around lived experience—offers a pathway toward that vision. By embedding peer services within a broader collaborative digital environment, organizations can enhance continuity, strengthen retention, and align technology with recovery principles.
Ultimately, digital transformation in behavioral health should not be about sophistication. It should be about support.
When technology reflects the realities of the recovery journey—its nonlinear progress, its vulnerable transitions, its need for human connection—it becomes more than infrastructure. It becomes a bridge between visits, between people, and between access and engagement.
Jorge R. Petit, MD, is a Behavioral Healthcare Leader, Author, and Founder/CEO of Quality Healthcare Solutions, LLC. Dr. Petit is the Chief Clinical Advisor at Cantata Health Solutions, a leading provider of technology solutions for behavioral health and human services, providing strategic clinical guidance on behavioral health integration, and technology-enabled care delivery. Dr. Petit is also a long-time Board Member and past Chair of Mental Health News Education, the publisher of Autism Spectrum News and Behavioral Health News. For more information, visit his website: www.drjpetit.org, blog: Behavioral Health: Matters, LinkedIn: Dr. Jorge Petit, MD, or Substack: drjrpetit.substack.com.
Matt Kudish, LMSW, MPA, is a behavioral health consultant, advocate, and Founder of We Better Work LLC. He serves as a consumer advocacy consultant at Cantata Health Solutions, where he provides strategic guidance on consumer engagement, digital health design, and peer-informed technology development. Matt previously served as CEO of NAMI-NYC, where he led the organization through a period of significant growth and systems-level advocacy. For more information, visit WeBetter.Work or LinkedIn: Matt Kudish.
Footnotes
- Solomon, P. (2004). Peer Support/Peer Provided Services Underlying Processes, Benefits, and Critical Ingredients. Psychiatric Rehabilitation Journal, 27(4), 392–401. https://doi.org/10.2975/27.2004.392.401





