Behavioral health best practice incorporates a whole-health perspective that emphasizes wellness, is person-centered, and focuses on the whole person and their strengths, not their illness (Swarbrick, 2006). Occupational wellness, that “personal satisfaction and enrichment derived from one’s work” (SAMHSA, 2012), is key to identity for many. Not finding employment can be a barrier to achieving wellness and even a roadblock on the recovery journey. Community Care Behavioral Health Organization (Community Care), a nonprofit behavioral health managed care organization part of the UPMC Insurance Services Division, encourages exploring employment as part of recovery-oriented care and has developed supportive resources for practitioners and individuals returning to work.
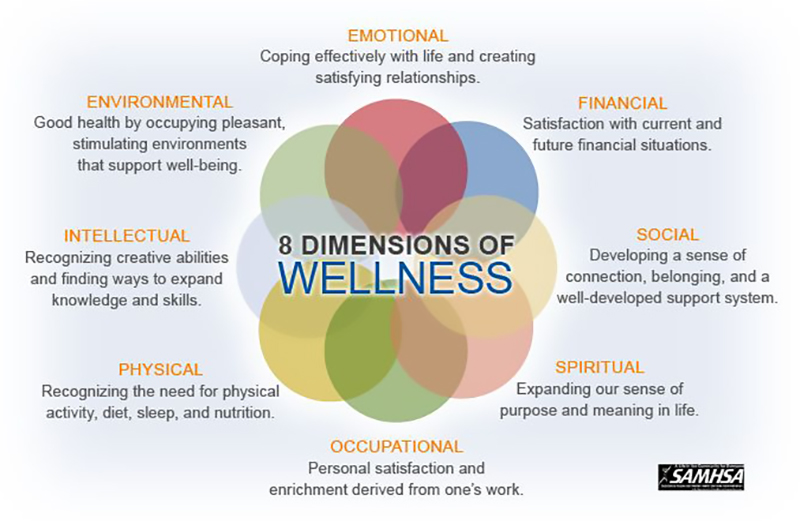
SAMHSA’s Eight Dimensions of Wellness (SAMHSA, 2012)
Viewing Disability Benefits through a Whole Person Wellness Lens
When individuals in recovery cannot work, they are encouraged to apply for income support programs such as Social Security Disability benefits (SSI, SSDI) and associated health insurance (Medicaid, Medicare). Applications for these benefits require people to provide evidence that they cannot work due to a medical condition, and initial denials, appeals, and reapplications are the norm. Working and earning money during this period, which may take years, may jeopardize receiving benefits.
Eligibility to receive disability benefits also requires a person to define themselves as a “patient,” assuming a “sick” identity that can erode self-confidence and increase feelings of worthlessness (Brice, 2018; Yanos, Roe, & Lysaker, 2010). Once approved for benefits, the individual starts receiving money as long as they are ill and unable to work, potentially disincentivizing some who want to work.
It is widely known that, like mental illness, long-term unemployment is associated with lower self-esteem and motivation, poor physical and mental health, increased substance use, and social isolation (Marrone & Golowka, 1999; Marrone & Swarbrick, 2020). Employment can potentially support financial, social, emotional, mental, and physical wellness for some with behavioral health conditions. At Community Care, we view employment as a potential tool in the recovery journey toolbox and encourage the exploration of work for individuals in recovery-oriented care.
Exploring Employment’s Healing Potential in the Recovery Journey
Employment can be a critical motivator for recovery, and individuals can work if they have the interest, the skills for the job, and adequate medical and social support. At Community Care, we have witnessed employment empower individuals to use their strengths, actively participate in choosing a direction for their lives, and engage their team to support their recovery journey.
In addition to being foundational to a new identity, work can enhance one’s self-esteem and reveal skills and talents that may have been dormant for years. Revisiting work with support may be a powerful tool for moving forward if work was a past source of stress or not an experience the individual may have had. Belonging to a workplace can impact social and emotional wellness and promote social connections and relationships – for many, friends are people met at work. Achieving employment goals may also provide purpose and meaning to individuals and those around them. Peer specialist colleagues who have experienced recovery and successfully returned to the workforce to serve as supportive role models can find personal fulfillment through their work. One peer specialist shared: “Working gave me a reason to get out of bed in the morning. It’s so rewarding to support someone else to move ahead in their recovery by going back to work.”
Addressing Challenges to Focusing on Employment
Working, even when positive and desired, can be stressful, and managing that stress is paramount to fostering wellness and promoting the positive impact of employment. Community Care offers digital resources for members to navigate stress and promote wellness, such as Self-Management Articles developed by Pat Deegan & Associates, the Academy & Library, and the new RxWell app, which includes on-demand and ongoing supportive health coaching to address depression, anxiety, and healthy living.
For people receiving SSI and SSDI benefits, worries about losing these benefits can be a barrier to exploring work as the rules about working are complex and may be difficult to understand. Community Care’s Working with Benefits webpage offers a compilation of resources for both members and providers that includes a provider Toolkit and training that demystifies this process and supports the transition to work.
Shifting Wellness and Workforce Paradigms and the Ripple Effect of Working
Work can support and enhance recovery, and employment has the potential to produce a ripple effect, improving other domains of wellness. Changing identity to a valued social role, from patient to employee, can impact emotional wellness. The working person has more money to spend on environmental wellness essentials like safe housing and transportation, healthy food and health care services that support physical wellness, and other expenses like leisure, education, and creative pursuits that influence intellectual wellness. Having a place to “belong” and new social connections fosters social wellness.
In addition to personal benefits, encouraging people with behavioral health conditions to work also benefits others and society. People with lived experience of recovery diversify our workforce with their unique talents and perspectives. They inform health care programs and services. Community Care employs people with lived recovery experience as Peer Recovery Support Specialists and in all levels/positions – leadership, direct care, and business operations. At Community Care, we believe that employment is essential in an individual’s journey toward recovery and wellness and that working works!
Kim L. MacDonald-Wilson, ScD, CPRP, is the Senior Program Director of Recovery and Wellness for Community Care Behavioral Health, UPMC Insurance Services Division and Adjunct Assistant Professor of Psychiatry at the University of Pittsburgh. Tracy A. Carney, CPS, CPRP, is a senior recovery/resiliency specialist at Community Care Behavioral Health.
References
Brice, G.H., Jr. (2018). Wellness benefits of a Social Security exit plan. Psychiatric Services, 69(3), 257-258.
Marrone, J., & Golowka, E. (1999). If work makes people with mental illness sick, what do unemployment, poverty, and social isolation cause? Psychiatric Rehabilitation Journal, 23(2), 187-193.
Marrone, J., & Swarbrick, M. (2020). Long-term unemployment: A social determinant unaddressed within community behavioral health programs. Psychiatric Services, 71(7), 745-748.
SAMHSA (2012). SAMHSA’s Wellness Initiative: Eight Dimensions of Wellness. HHS Pub. No. (SMA) 12-4958.
Swarbrick, M. (2006). A wellness approach. Psychiatric Rehabilitation Journal, 29(4), 311-314.
Yanos, P.T., Roe, D., & Lysaker, P.H. (2010). The impact of illness identity on recovery from severe mental illness. American Journal of Psychiatric Rehabilitation, 13, 73-93.





