Access to actionable data makes for smarter decisions and leads to better outcomes. Healthcare providers readily acknowledge that more targeted services are possible when armed with real-time, client specific information. There are many sources of data, including but not limited to electronic health records (EHRs), health information exchanges (HIEs), payers, government partners, strategic vendors offering client facing services (e.g., client transportation), and a multitude of agency developed tracking forms. Arguably, the challenge is not lack of data but, to the contrary, too much data stored and presented in a disorganized and ultimately unusable format. IMSNY’s core product, DABI (standing for Data Analytics Business Intelligence) solves for this in a groundbreaking manner, leveraging the powerful analytics capability of Arcadia1 combined with subject matter experts from two of the largest behavioral health Independent Practice Associations (IPA) in New York.
Before diving into the solution, it is important to clearly identify why analyzing data is important. The quadruple aim is the guiding principle for healthcare delivery, and focuses on improving the client experience, achieving better total health for the entire population, reducing the cost of healthcare, and optimizing the well-being of the “care team.” Without clearly presented data detailing what is happening with the client population, progress is difficult to measure. Conversely, if a service provider has the data to predict when a client is at risk, timely intervention is possible. For example, an expensive inpatient stay could be avoided by implementing an effective community intervention at the right time, thereby improving the client’s life and reducing cost to the system.2

Figure 1: List of Data Points and Sources
For a data analytics solution to be useful, it needs to have the ability to perform complex analysis with customized algorithms. The information returned to the network or to the provider must be easy to digest and speak to the needs of the population served. For example, knowing the percentage of a specific population that speaks Spanish as their primary language offers insight that a behavioral health provider can react to and make decisions based on (like hiring more Spanish speaking therapists). IMSNY and Arcadia have access to a huge set of publicly available data that can greatly impact care delivery, and when matched with specific client data sourced from Figure 1 a 360° view of a client is possible. This leads to better point of care decisions as well as a coordinated network response to more pronounced population health needs.
Healthcare networks all share the same overarching goal of improving the health of their clients. There is a host of specific measures to track, each requiring a different intervention. An IPA or similar provider network is required to build out a set of behaviors or health targets that it wants to improve, determine interventions that impact outcomes, and then track how effective the interventions are over time. IMSNY’s two founding IPA networks chose to focus on eighteen specific priority health measures, each one with a specific “target track.” A target track, in this case, is a structured map of activities that a provider network uses to guide activities to impact a specific measure. By using a consistent intervention, or “track,” fidelity to a specific process is maintained allowing for better cause and effect analysis. See Figure 3, which shows the target track for Follow Up: Post Inpatient Hospitalization. This and seventeen other measures were chosen in partnership with the CBC and CBHS IPA clinical quality committees, comprised of representatives from 80+ agencies. By tracking, reporting, and building interventions around many of these, the network expects to see health improvements and reduction in negative health outcomes (e.g., avoidable emergency department use).

Figure 2: IMSNY BH Priority Measures – sampling
A useful exercise when putting together a system for data analytics is to carefully review a target track and determine how to secure data for each node on the map. Using Figure 3 as an example, the first data point for DABI to track is the occurrence of an inpatient hospital stay, which IMSNY learns of through its partnership with a Health Information Exchange (HIE).3 As this track is focused exclusively on whether a client attends a follow-up appointment, the subsequent nodes are tracked through direct connections to network agencies’ electronic health record or billing files, which contain details regarding appointment status. IMSNY ingests this data and reports gaps in care. By following an agreed upon, standardized intervention and pulling this information into DABI, the network can effectively track progress on each measure and share associated data with agencies providing point of care services.
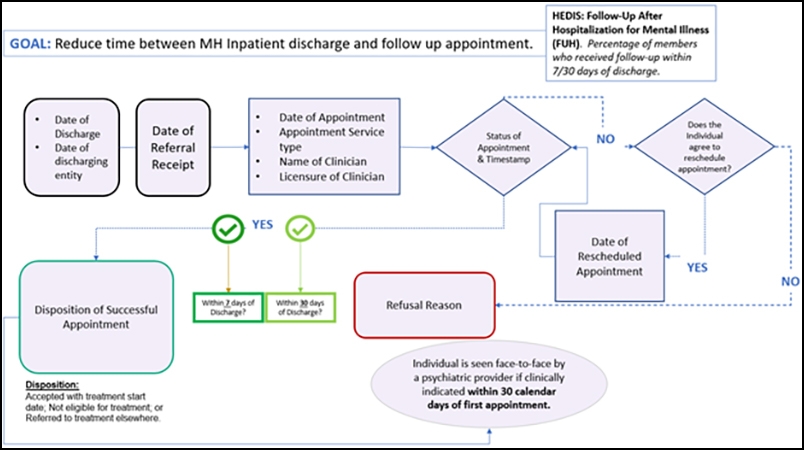
Figure 3: Target Track – FUH 7/30 day
DABI – Our Solution
Innovative Management Solutions of New York (IMSNY), a joint venture between two of the largest behavioral health IPAs in New York, aggregates and analyzes data from sources that have been historically challenging to access, allowing for insights that impact how care is delivered. Substance use disorders and mental health conditions play critical roles in overall population health but are often underrepresented through the lens of claims data alone. Our solution includes not only claims data, but ADT (admission, discharge, transfer) feeds from Health Information Exchanges (HIE), Electronic Health Records (EHRs), and social determinants of health data sources, allowing for a full understanding of what is “happening” to the clients served through either an agency-specific or total-network view.
DABI aggregates, normalizes, and analyzes data, with clinical experts overseeing the quality and outputs to ensure that they result in actionable insights that lead to improved workflows, processes, and consequent health and quality of life outcomes. What makes the platform unique is its focus on behavioral health and social determinants of health-related measures, viewing these factors as critical drivers of optimal total health in a value-based payment context.
Once data sources are normalized (i.e., made to conform to a format that can be understood by an analytics platform), they are fed to Arcadia. By hooking into Arcadia’s engine, IMSNY’s IPA networks can seamlessly track and make decisions based not only on the sum of contributed data sets, but also leveraging a multitude of layered-on databases (e.g., census data) and proprietary algorithms that allow for risk stratification.
While the Arcadia solution represents the most pronounced value to participating networks, there are intermediary tools developed by IMSNY to support participating networks immediately. In partnership with MD Health, IMSNY created a tool to organize and present data from billing files. Using this tool, IMSNY aggregated files from 30+ agencies in NYC and the Hudson Valley with the goal of delivering immediate insights about not only their individual billing files, but how they compare to others in the network. A While the Arcadia solution represents the most pronounced value to participating networks, there are intermediary tools developed by IMSNY to support participating networks immediately. In partnership with MD Health, IMSNY created a tool to organize and present data from billing files. Using this tool, IMSNY aggregated files from 30+ agencies in NYC and the Hudson Valley with the goal of delivering immediate insights about not only their individual billing files, but how they compare to others in the network. Whether their mix of diagnoses is aligned with the rest of the network, or if they are treating a different mix of clients. Using this data, an agency can determine whether to further customize service offerings to meet the unique needs of their clients.
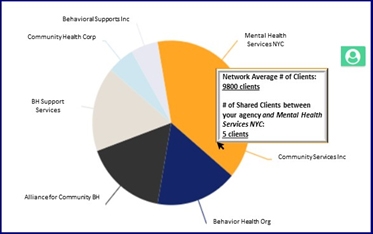
Figure 4: Clients Shared Among Network Agencies
Additionally, the solution shows agencies which other in-network agencies they are sharing clients with, giving valuable intelligence around which agencies they could more closely partner with. (see Figure 4)
Looking Ahead
With the availability of data, made possible by the advent of electronic health records and other technology platforms, failing to make decisions informed by all accessible information is increasingly irresponsible. Furthermore, in a value based contracting environment, payers may cease to contract with networks that do not have a sound method for tracking network activities and consequent health outcomes. With DABI, IMSNY has developed a system for combining complex data into a singular, easily reportable data warehouse. More importantly, IMSNY is breaking ground with Arcadia by jointly developing behavioral health functionality, as most analytics platforms have only designed their algorithms for physical health outcomes. Through this partnership, IMSNY and its affiliated networks will continue to advance the mission of improving access to health data, and helping providers make better decisions to improve population health.
IMSNY’s affiliated networks include over 80 agencies serving nearly 160,000 people in the Hudson Valley and NYC, all of which are committed to supporting this solution and are looking to DABI to improve the system of care and engage in meaningful VBP contracting with payers.
IMSNY’s Parent Companies
CBC was launched in 2011 by innovative NYC not-for-profit behavioral health agencies to meaningfully participate in NYS’s Medicaid redesign and Value Based Purchasing initiatives. In the following years CBC developed a citywide Health Home, which is currently the largest of its type in New York State. CBC has launched effective gap-filling service programs for low-income New Yorkers that build on the expertise of its community-based service network. CBC “knits together” affiliated agencies to holistically address treatment and recovery needs, while assessing community deficiencies and connecting clients to needed support.
CBHS realizes the need for nimble, responsive, cost effective ways to serve people with behavioral health other related challenges. To accelerate their knowledge and preparation for value-based contracting, CBHS partners with healthcare agencies, health homes, and managed care companies to achieve the outcomes needed for a healthier future. CBHS is creating an array of innovative services that are financially viable and responsive to the needs of the clients served. CBHS has been a leader in New York State’s transformation to a person-centered model of care and is recognized for its recovery services, which are outcome-driven and incorporate peer and natural supports. CBHS utilizes strength-based planning in the behavioral health and child welfare services that draws heavily upon community supports to promote positive outcomes.
Jorge R. Petit, MD (Co-CEO), Mathew Smith (COO), and Khushi Shah (Data Solutions Manager) are at IMSNY, focused on supporting behavioral health networks. To connect, reach out to msmith@imsnyhealth.com.
Footnotes
- Arcadia is a healthcare data and software company dedicated to healthcare organizations achieving financial success in value-based care. Arcadia Analytics, their purpose-built population health platform, delivers enterprise-level transformational healthcare outcomes.
- To learn more about CBC’s Pathway Home program: Pathway Home™ – CBC (cbcare.org)
- IMSNY partnered with HealtheConnections, see press release



